Depression is a major human blight. Globally, it is responsible for more ‘years lost’ to disability than any other condition. But the pathophysiology mechanisms of depression is not very clear and the most common antidepressants are still targeted the monoamine neurotransmitters sine 1950s. Yet depression is widely undiagnosed and untreated and half of the patients who received therapy cannot get help from current treatment. All of these called scientists to find new way to cure depression. Prof. JIN Feng and his team from Institute of Psychology, Chinese Academy of Sciences, have studied the relationship between gut microbiota and behavior since 2003. They found that the mammals’ behavior and emotion were closely connected with gut microbiota. Through the microbiota–gut–brain axis, the brain can influence gut bacteria by modulating gut physiological status, and the composition and variation of intestinal microbiota can change the central nervous system and behavior. And regulating gut microbiota through probiotics supplementation could make effect in many behavior disorders, including depression, anxiety, autism, schizophrenia, etc. Dr. LIANG Shan and her colleagues in JIN’s team designed an animal research using chronic restraint stress model and obtained several interesting foundlings. Chronic treatment with probiotic Lactobacillus helveticus NS8 during restraint stress demonstrated anxiolytic and antidepressant effects, promoted cognition, decreased plasma CORT and ACTH levels, modulated pro-inflammatory and anti-inflammatory balance, meanwhile restored 5-HT, NE, and BDNF content in the hippocampus, inducing an effect better than that of SSRI. These data confirmed and demonstrated the hypothesis that probiotic supplementation may be an effective and safe therapy for chronic-stress-induced depression. The study was granted by NS Bio Japan and NS Bio Guangzhou. The article has been published on Neuroscience. 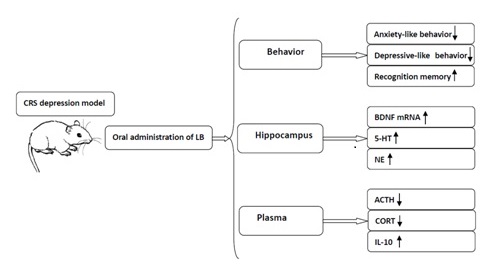
Fig. 1.Graphical abstract 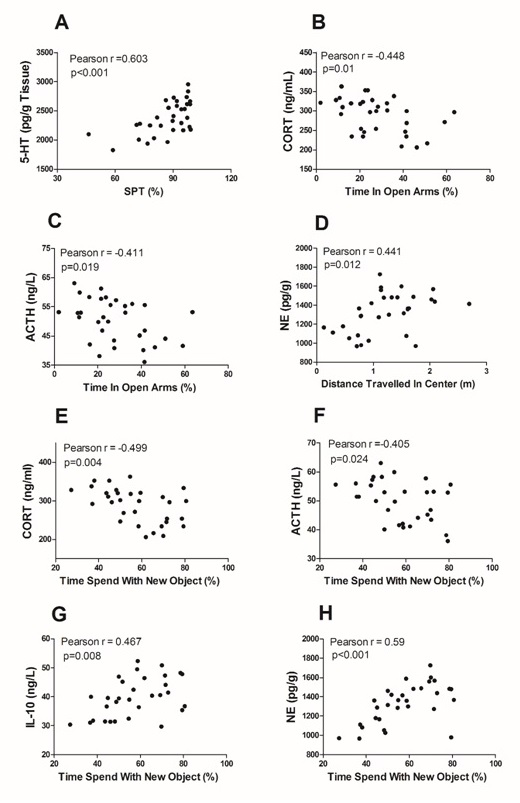
Fig. 2. The behavioral results were correlated with relevant biological outcomes. Panel A shows the correlation between sucrose preferences and hippocampus 5-HT content. Panel B and panel C show the correlation between time in open arms in EPM and plasma CORT and ACTH levels. Panel D shows the correlation between distance traveled in center in OFT and hippocampus NE content. Panel E, panel F, panel G and panel H show the correlation between time spend with new object in ORT and plasma CORT, plasma ACTH, plasma IL-10 and hippocampus NE content, respectively.
Related Articles: Hu, X., Wang, T., Liang, S., Li, W., Wu, X., & Jin, F. (2015). Antibiotic-induced imbalances in gut microbiota aggravates cholesterol accumulation and liver injuries in rats fed a high-cholesterol diet. Appl Microbiol Biotechnol, 99(21), 9111-9122. doi: 10.1007/s00253-015-6753-4 Wang, T., Hu, X., Liang, S., Li, W., Wu, X., Wang, L., & Jin, F. (2015). Lactobacillus fermentum NS9 restores the antibiotic induced physiological and psychological abnormalities in rats. Benef Microbes, 6(5), 707-717. doi: 10.3920/BM2014.0177 Hu, X., Wang, T., Luo, J., Liang, S., Li, W., Wu, X., . . . Wang, L. (2014). Age-dependent effect of high cholesterol diets on anxiety-like behavior in elevated plus maze test in rats. Behavioral and Brain Functions, 10, 30. doi: 10.1186/1744-9081-10-30 Luo, J., Wang, T., Liang, S., Hu, X., Li, W., & Jin, F. (2014). Ingestion of Lactobacillus strain reduces anxiety and improves cognitive function in the hyperammonemia rat. Sci China Life Sci, 57(3), 327-335. doi: 10.1007/s11427-014-4615-4 |
